Well, why not? I want to and I can.
Many people question my rationale as to why I do so much exercise, particularly whilst being on TPN. Honestly? There are so many reasons, some personal, others less so.
Number 1 is probably the most crucial sport/ exercise makes me feel good. It helps keep me strong physically, provides great escapism, and is fantastic for my mental well-being.
I think that being fit and as healthy as possible is what helps me avoid so many complications and is great for symptom management. On paper, I shouldn’t be as able as I am, but I work hard to keep strong and it seems to pay dividends.
It gives me purpose and drive, things that are so often lost with chronic health problems.
I have a reason to get out of bed every day, something to work towards. The goal constantly evolves – doing the same exercise faster, or with a heavier weight etc… it’s never completed.
I can definitely tell the difference when I’ve not been training. I am fatigued whether I train or not, but the fatigue I experience from exercise ensures I sleep well and as a result helps me manage my underlying fatigue.
It is of course a balancing act. It is imperative I listen to my body, if it’s screaming for more sleep then that’s what it gets. If I have horrific DOMs then I adjust that day’s session to manage it. If my gastro symptoms are flaring, I focus on managing them. It’s the same for any athlete, you learn to adapt and respond to what you’re feeling. For me with unstable health, it’s an invaluable skill, it means I’m aware of when things are straying from my ‘normal’, and I can be proactive about my health.
It’s also a lesson in time management, trying to fit my degree, my training, medical treatments, appointments etc.… into the day or week, without overloading it and skipping important things like rest periods as well as everything that goes into being an adult aka paperwork!!
It’s also a learning experience, there’s more to any sport than just being able to do it. You need to master the skills, practice the smallest movements until you don’t have to think about them, learn how to manage pre-competition nerves, performance anxiety, and how to remain focussed during an event and training sessions. A major competition could be years away, but you have to give your all every training session as that can be the difference between Gold and Silver come match day.
You also learn how to manage setbacks, bad sessions, poor results, and injuries, working out how to continue contributing to your goals even if you can’t train like usual.
These are very handy tools for life, whether you have a disability to manage or not.
Away from personal development and enjoyment, there is the challenging of assumptions.
I once sat at a Gala Dinner celebration post International race and during a conversation with a newly qualified dietitian, she said to me, but you can’t row if you’re on TPN. I replied that she’d seen me compete therefore it must be possible. She reconsidered her stance and said it shouldn’t be possible. When I asked her why, she said that we are meant to be too sick. I explained that the point of TPN was to facilitate me living, and that there were many people doing extraordinary things on TPN. We spoke some more and she said she was going to talk to her colleagues about me, to make sure everyone was helping their TPN patients live their dreams, and if she worked in that field in the future she’d tell her patients about me.
This isn’t about boasting or showing off, this is much more important; this is about raising awareness in the purest way, by being in the community, by taking these chance meetings to show what is possible. If my actions encourage someone else to follow their dreams, I will be ecstatic.
“Something is only impossible, until somebody makes it happen”.
It’s not just about encouraging people on TPN to be more active, it’s about the positive impact exercise, and movement can have on everyone, particularly those with chronic illnesses.
I believe so deeply in the power of movement for recovery. It can be difficult knowing how to start becoming more active again, and this is something I would really like to help people with. I would like to enable those who want to become more active learn a safe and effective way of facilitating their goals.
Many people have been exposed to bad advice, either from physiotherapists, Doctors, the Internet, other people with their condition(s), and ‘well meaning’ family and friends. This can destroy their confidence and make people unsure how to take the first steps into a more active lifestyle.
The key thing is that it needs to be person specific and targeted appropriately.
The benefits of physical activity are numerous and I want to show and help people realise that it is possible and important to become more active despite your health problems. There are so many myths to dispel and barriers to break down as part of this. Many people want quick fixes to control their symptoms, whereas physical activity has been shown to help manage so many conditions. I’m not for one minute suggesting throwing away medications, but that we need to be as proactive in helping ourselves as possible.
It is not a cure, but like many things, it’s a management tool.
That’s why I do sport.
So over a year has passed, where have I been?! Well I have been very scarily fighting for my life.
I’ll try to keep this short, but it’s a long story.
Last September, having a relatively good period of health, I’d taken my handcycle and gone on a three-hour coaching spree in the absolute pouring rain. I’ve been less wet in the bathtub!! Other than resembling a drowned rat, I was feeling absolutely fine. I warmed up, dried off etc… and went to bed.
The next morning was the beginning of the nightmare that has been the last 10 months. I woke with backache, nothing spectacular and not horrifically uncommon- I sit down all day and had spent 3 hours on my bike in the freezing cold, something was bound to hurt. The odd thing was that I couldn’t straighten up. Refusing to pay too much attention to this, I applied heat, convinced myself it was a bad muscle spasm, got medication from the GP, and arranged an emergency sports massage. As the day progressed the pain got worse, it wasn’t responding to heat, ice, pain meds, muscle relaxants etc.… I carried on though, as the day progressed I started shaking and not being able to bear my weight whilst sitting up, despite this I still coxed a crew, well it was that or they didn’t go out and I couldn’t bear that.
Things kept getting worse, I had to take the weight through my arms when sat, I still couldn’t move to an upright position, but still I denied a serious problem. The Calea nurse came and went, my carer came, and I insisted I wanted a shower (despite the shaking and severe pain thing). She insisted I sought medical attention so I messaged a medic friend of mine who replied with “You should have phoned an ambulance 6 hours ago”. Reluctantly I considered this, with her messaging every few minutes to check whether I’d phoned an ambulance.
With much reluctance, I gave up, and the carer phoned for help. I got a friend to come round as well. By this time I was just lying on the bed yelping. Still trying to convince myself it was just a muscle spasm and this was fuss over nothing.
Eventually the paramedics arrived, by which time things were getting a little hazy. I recall them walking in and thrusting Entonox at me without saying much. I think they could probably hear my yelps in the street. With plenty of Entonox on board, they managed to get some sense out of me.
I remember we did my basic obs; everything was fine bar the raging fever, which I hadn’t noticed at all. At this point, I remember saying, “Is this the time to tell you I have a central line?” Cue serious faces from them and checking I was serious. We rushed, very gently over to A&E, where I continued to consume copious amounts of Entonox.
The Doctors were fantastic. It was clear I had an infection and it was assumed I had a central line infection that had probably gone septic that was causing all the pain. They tried, but failed to follow sepsis protocol- I should have had a stat dose of IV Domestos before leaving ED, but they were too worried about me breaching to get it sorted. They also didn’t sort out my pain relief properly and left me screaming in agony all night.
I had started having huge back spasms that brought my knees to my chest. The plan was badly thought out and they decided to send me for a PICC before starting my PCA, by this point, my back was continually spasming and I was stuck, completely in the foetal position on my side, which made for PICC insertion difficult. They also failed to sort out my dignity – I was desperate for the bathroom at 5 AM, but couldn’t get on a bedpan for the aforementioned reasons. Eventually my team came and decided that I probably had a line infection and would be up and out of there in a week with some IV antibiotics, but they would do a spinal MRI just to make sure. The plan was to put an In-Out catheter in until the PCA started and I’d be able to move more easily. The ‘minor’ problem being no suitable catheters on the ward, and I think the world’s slowest walker went to the other side of the hospital to steal some from Urology. Then there was the faff that the nurses didn’t know how to use them, errmmm it’s a catheter it’s not that hard and you put Foley’s in regularly.
My bladder by this time was progressing from hill to small mountain and eventually got impatient, I won’t tell you the rest, but I was a very soggy and unhappy patient.
Eventually things were settled, I had the PICC placed so I could get some decent pain relief, I moved to my usual ward, but I was still having massive back spasms. Eventually someone added in some IV diazepam and I finally managed to start sleeping a bit better.
MRI day came, I was told off for moving too much- they’d taken away my pain relief as it was out of hours, and I hadn’t had any diazepam for hours. Eventually exhaustion hit and I fell asleep in the scanner.
Back on the ward, the next morning and hell really started to happen. The MRI showed I had a massive Paravertebral abscess from L4- base of sacrum, Discitis at L5/S1 and Osteomyelitis at the same point, as well as a few other bits and pieces. The question was what to do. They said they couldn’t biopsy because of all the nerves in the area, but the blood cultures were showing nothing. Therefore, we started chucking more antibiotics at it.
I just didn’t get better. After 2 weeks, I was still as bad clinically and my fevers hadn’t gone anywhere. More antibiotics were trialled, but after 5 weeks no change. A 6-week course of other antibiotics was embarked on. I was starting to turn a corner, the labs were looking better and my fevers were down. Then 5.5 weeks into the course fevers returned and my labs were off again. We extended for another 2 weeks, at point 7 weeks and 5 days having been fever free for nearly 2 weeks I spiked a massive fever. I told my consultant and she said it was just a one off and not to worry. Cue a whole day of fevers. I woke up the next morning and found my consultant at the end of the bed “I wasn’t expecting to see you today”, “well I wasn’t expecting you to have fevers all day” she retorted!! After a long discussion with Infectious Diseases, they decided a 12-week course was the answer.
Sometime during this experience, somebody decided that I might be having antibiotic fevers and they wanted to stop my antibiotics for 48 hours and see what happened. Part way through that experience I spiked an over 40°C which persisted for the whole day, at some point in the early hours of the morning I was woken by the Critical Care Outreach Team, one of the scariest points of the experience, they are NOT a good sign. Thankfully, I went back on to the antibiotics and the fever came down. I had a similar experience when they changed the antibiotics to one I told them never worked for me, and that didn’t go well either.
So having had 5 weeks of mix and match antibiotics I then had a 12 week course of IV Domestos (other brands of bleach are available).
Somehow, a week turned into 100 days, I don’t quite know where or how, but what I thought had been a couple of weeks had turned into several months.
Eventually my birthday loomed, yet another big birthday that was looking to be a disaster. People did their best. My Mum sent some 30 balloons, they were much larger than anyone ever expected and caused much amusement on the ward!!
They also let me use a meeting room to have a little party the weekend after my birthday. I was so grateful to everyone who came to make it a special day. I eventually crashed out and fell asleep in the party!!
Birthday joy (and the giant numbers!!):
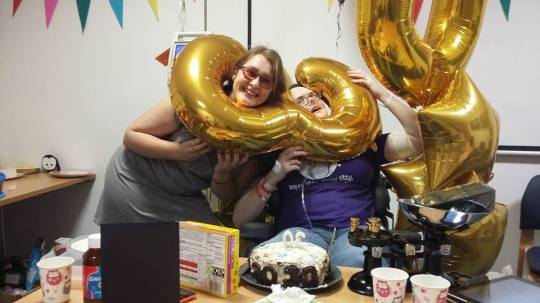
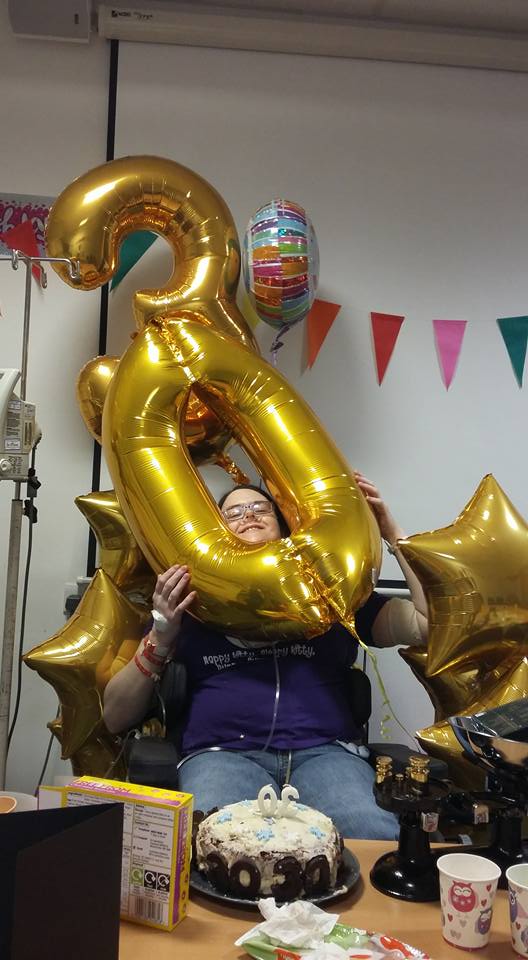
During all of these antibiotics, I had to undergo major physio- I couldn’t sit up to begin with and we did a lot of work to get me moving again. The first day they hoisted me out of bed I didn’t even make into the chair before I had to go back to bed again.
This was one of the hardest fights of my life. I was determined I wasn’t going home needing to use a hoist. Nope not happening, no way. (I have nothing against hoists as such, but I wasn’t letting this infection change my life even further). We battled a lot; there was a lot of tears, a lot of pain, but also a lot of laughter. I was fortunate enough to have the most amazing Physio and OT team. I don’t think I could have done it without them. They told me it was all my work, but they were there cheering me along, making me believe I could do it. I honestly think the outcome would have been different if it hadn’t been for them. Towards the end of my stay the physio changed and he was not at all supportive and I think would have made my recovery a lot less effective. Thankfully, by the time he was involved I was well on my way back to recovery.
My first time in a chair for months:
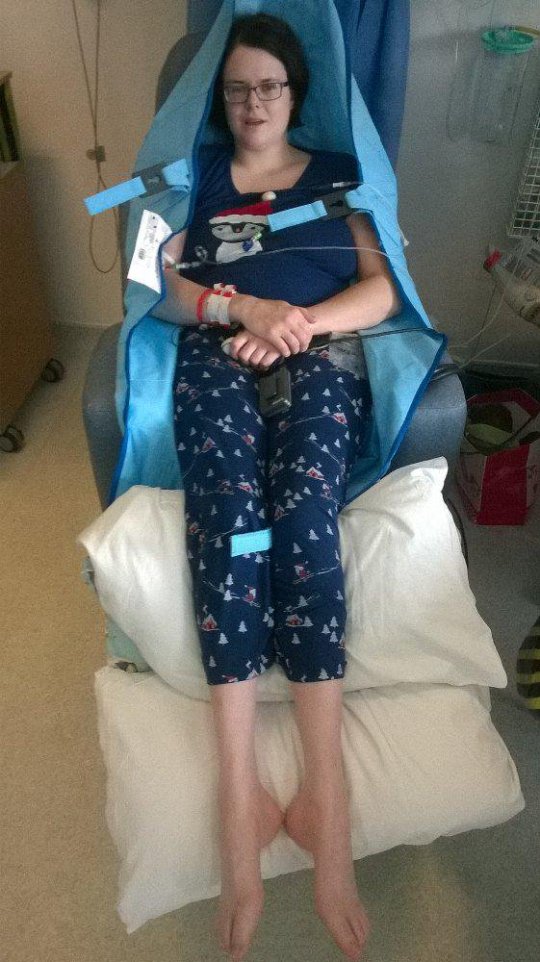
My first trip outside in even longer:

Shortly after my birthday came Christmas. Hospital Santa left me a nice present, and I was allowed a few hours home with my parents. We made the best of it as we could, but I eventually hit a wall and needed to go back.
I got to play with my beautiful gerbils though, who I hadn’t seen since September, and I’d only had them about 3 weeks before I went in, but, they seemed to know who I was and were very well behaved.
I spent Boxing Day recovering in hospital and slowly opening some more presents. I learnt Santa is extra generous when you’ve been fighting for your life!! The next day I got a few more hours leave and went home again. I had to wade through masses of paperwork and try to get some sort of semblance of normality going on. There were more presents (yay!!) and then back to recovering at hospital.
Eventually I started being able to get more independence. I still couldn’t sit up straight, and was stuck in a huge wheelchair, which reclined and tilted in space, which was fantastic at the time.
During this time, I was also assessed for Continuing Healthcare to try to get me more support at home. I had to prove that my needs were mostly medical rather than social, and that they fulfilled a few other criteria. A lot of stress, a lot of paperwork and unpleasant experiences accompanied that, but eventually I was approved.
I was to be sent home with 24/7 live- in care. This was a huge shock and is still taking adjustment. It also meant I had to sort out the spare room as it was basically a junk room, and we had to make it habitable somehow. Fortunately, just before I went in some friends and I had cleared the room a bit so that the gerbils could live in there, and people could stay the night at a pinch.
There was still a lot of work to do to make it habitable though.
By now, it was February and I was finally off my antibiotics, but still under the care of the Physio and OT and still trying to sort out the care arrangements.
I was given weekend leave, which was exciting and a big step forwards (and a huge one back as well as I was to discover). I was chief delegator whilst sat on the sofa. Eventually I fell asleep, I woke up shivering. I assumed I was just not used to the normal temperature of my house rather than the Greenhouse of the hospital. I was due to go to a formal meal and then a meeting the next day, which is why I choose that weekend for leave.
I continued to shiver despite a warm bath and many layers. I headed off to my dinner regardless (Denial is fantastic!!) Eventually I stopped shivering and didn’t think much of it. The next morning I woke feeling okay, and then all of a sudden the Rigors hit again. I was vomiting and apparently looked horrific. I was adamant I was going to my meeting, and then all of a sudden it hit me and I was desperate to go back to the hospital to sleep.
On arrival, we mentioned it all to the nurses, and I had a raging 41°C fever. ‘Flu had just hit the hospital and was about to hit the ward, so it was assumed that was the problem, and we would continue with preparations for discharge on Tuesday. They took some blood cultures just in case, but my primary consultant had just gone off sick too, so it was assumed to be one and the same having spent an hour or so talking to him on the Friday.
We continued planning for discharge, being reassured again it was just ‘flu, and then a nurse asked me why I was being started on IV antibiotics. I had no idea and we thought maybe it was a clerical error; suddenly a Doctor appeared and explained that I had sepsis again. This time they’d grown a bug so they knew what to treat. This was a kick in the teeth; having already had 17 weeks of Vancomycin my body wasn’t keen on more. To add to the joy I also managed to contract MRSA and got myself moved to a side room.
I redecorated the room with all the amazing cards and letters that my friends had sent. I couldn’t believe the amount of support I’d had over the last five and a bit months.
The Wall Of Love (several layers deep in places):

Another 2 weeks of IV Domestos and I was ready to go home. It was a new world I was going into, my hopes and dreams had been crushed (that’s for another post), and someone was going to be with me 24/7. For a creature of isolation, this was going to be a big change.
I made it 5 days and then aspirated vomit into my lungs. Having done a sputum sample I’d grown some nasty bugs and needed some IV antibiotics to treat it. 10 days after spending over 6 months in hospital, I was being readmitted. This was to be a simple couple of days impatient so that I could pass my test to treat at home. This, however, being me meant things didn’t quite go that way. What I hadn’t been told on admission was that my kidney function had gone awry. I continued with treatment and then one day I started becoming really drowsy and unresponsive. The nurses weren’t worried and thought I’d just had too many of my drugs. I was in a state; I was very distressed, as I couldn’t work out what was happening and why I couldn’t stay awake etc… The night team came on and the HCA went ape, she demanded a Doctor came to see me immediately I was completely different to the night before.
The doctor came and informed me that my kidney function had deteriorated even further, and that I had nephrotoxicity because of the opiates and benzodiazepines I was taking. She started treatment for that and kept an eye on me over night and into the morning. Around the same time, I’d had a bag of TPN and started feeling increasingly unwell. My obs were further off, and my central line tunnel was very swollen and painful. I’d become septic for a third time, despite already being on strong IV antibiotics. My heart rate slowed right down, my body was struggling, and I was actually very scared. Thankfully, with aggressive treatment things have recovered – my heart rate is still very slow at random, points and my kidney function is not completely back to normal. I have kidney pain now from the Acute Kidney Injury, but I’m hoping in time that will change.
I was eventually stabilised and managed to get home, but things have been rough since then. Having gone into hospital in September it was now April and I’d fought for my life three times in six months, lost my hopes and dreams, and had a completely new lifestyle to work with. I have permanent back damage, and have only just started managing to sit up straight again.
My life changed majorly and it was one of the scariest and exhausting experiences of my life.
Where I go from here unknown, and is definitely for another post.
If you’ve managed to get this far, I’m very impressed and I’m sorry it’s so long, but for an 8 month long rollercoaster ride from hell I’ve done my best to condense it. Thank you for your efforts, and of course to everyone who supported me during this hell.
Training has been going rather well recently, I’m not as fast as I’d like, but then what athlete ever is!? But my endurance is improving, and with that should come speed, so fingers crossed it is on the right path.
I’ve been trying to look at the nutrition aspect of my training recently. This of course is a very complex area for me given that I can’t tolerate much food orally and only absorb part of what I do manage to tolerate. Both my gastrointestinal team and respiratory teams have some involvement in my nutrition, the latter because of my reflux affecting my lungs. Each have an opinion about what should and shouldn’t be done, and me being me, generally have a different plan to both of them!!
Whilst they argue it out, I’m focussing on the basics- hydration during the day being the biggest, and the focus today. I get my primary fluids overnight in my IV bag, and can only tolerate around 300ml of oral fluid a day. So I need to make that 300ml contain the most value it can. I need to consider what I need, what I can tolerate and what I have planned for the rest of the day and the next days. I can rehydrate effectively day to day with my IV fluids, but trying to quench a post-training thirst, or rehydrate after a sweaty first session are not so easy to do. It’s not practical, nor safe to hook up extra IV fluids every day due to access and de-accecessing requirements. I will do it if it’s a dire emergency but it’s not ideal in any way (for my personal situation).
Some things I tolerate better than others, and at different times I tolerate different things. Generally water is the fluid I struggle most with, so I have to avoid drinking pure water. Instead if it’s just for rehydration as opposed to for refuelling, I’ll use an electrolyte tablet added to water, as I tolerate this reasonably well. If I need calories as well as electrolytes I’ll use a carbohydrate powder mixed in and for ‘Recovery’ I’ll use a protein/carb mix, but I find that hard to digest so tend to only use that on evenings.
I am pretty obsessed with fluid balances, output/input etc as well as weight. Dehydration is known to have a massive impact on performance not only physically, but mentally. A quick search produces thousands of articles discussing the negative impact it has, as well as hopefully mentioning the dangers of overhydration, so I’ll skip the details. Dehydration also affects one of my other health problems, so I have to be extra careful- I’m still learning though, and for me it’s not an exact science as so many other things affect my stomach and its ability to tolerate oral fluids. My days of glugging down a big glass of ice cold juice are well over, although I dream of this on a hot evening, because if I over do the fluids I end up with them coming back up, and my hydration levels worse than they were before I started.
Unfortunately with the summer coming, things get that bit more complicated, as I need to find some way of getting in extra day time fluids without being able to increase what I put in. It’s difficult and we’re still balancing it out, but now I have a second line in, I can piggy-back fluids to run with TPN, without it taking any longer. I’m hoping that this will work, this is the first year I’ve tried this so fingers crossed it works out okay. The risk with this is that I end up with fluid overload and best case scenario end up taking a lot of loo breaks, the worst case heart failure. So it’s a delicate balance!!
The downside to there not being people around who have tried this before, means you’re kind of on your own out there. It’s a work in progress, and I’m hoping to work with a sports nutritionist soon, so he might have some ideas, but due to the circumstances has never worked with a TPN athlete before- at least he should know the basic nutritional stuff, I just go with common sense and try and make some educated judgement calls.
It’s now less than a week to Henley Women’s Regatta, so I’m started to plan my fluid options for that. Thankfully I’ve only got the one race, so it’s easier in terms of hydration than last year, but is very much weather dependent and based on pre-planning estimates.
Hopefully it’ll work out okay and I’ll be a nicely pre-hydrated, ready to kick butt on Sunday!!
That’s the reality. Three years ago I started TPN, it saved my life, and completely revolutionised it.
I wrote extensively on this topic 2 years ago here: https://rowrowyourboat.wordpress.com/2013/06/01/365-little-days-later-why-pinnt-means-so-much-to-me/
Now I am back, this time to talk about fundraising for them. They’ve stuck by me as every challenge has cropped up, have introduced me to some fantastic friends and some random people who I love dearly. I have three years of additional life to celebrate, and I have definitely done some living in those years.
On Sunday I take on the Bupa Westminster Mile- don’t worry I haven’t suddenly learnt to walk, I took up wheelchair racing as part of my cross-training, so I thought why not give it a go?! It’s time to repay the favour, to ensure they can continue their fabulous work, plus I get to race (can take the rower off the water, but can’t take the racing mentality away!!).
I only started training for wheelchair racing in February and much has been punctuated by niggles and meetings getting in the way, so I’ve not had many sessions, and seem to have the worrying knack of tipping my chair, including in my first ever race!!
I’ve now done 2 competitions and 7 events across those, I’m not fast, but I’m having fun- although I have collected 5 medals and a third place out of those.
I hope anyone reading this will take time to read my fundraising page http://www.virginmoneygiving.com/claireconnon where I wax lyrical about the work PINNT do, and consider sharing and supporting this fantastic charity and my crazy endeavour!!
It’s feeding tube awareness week, feeding tubes are something close to my heart, quite literally!! , but do we really need to raise awareness of them? Now I’m aware this post may be controversial and in an ideal world, no one would bat an eyelid when you flash your belly for food/meds/venting, but I’m not sure raising awareness is the right way to go about it.
Most people will never come across directly someone with a feeding tube, so I wonder if it’s not the most productive use of time and energy, as most will probably disregard any info they see about it. Plus what does raising awareness actually do? We don’t need people to be aware of them, we need to educate about the realities, and the positives to them. I personally believe that the best way to do this is to get people you know talking about it. Just posting on the Internet is a bit of an abstract way to do this. There’s nothing tangible seeing photos and messages on the Internet, it needs a much more grass roots approach.
I will talk freely about my nutrition problems when it comes up in conversations etc.. People can ask questions without any prejudice and they learn, they aren’t any more aware of them as such, but have a better understanding of artificial feeding, and hopefully when they come across it again, they treat it as completely normal.
I think part of my dislike of raising awareness is that I hate some of the terminology surrounding it. The *word* “tubie” is awful. I find it dehumanising, it reduces a person down to not even their medical condition, but down to a piece of plastic that’s keeping them alive. I particularly hate it used in the phrase “I love a tubie”, no you love a person being kept alive by a tube, there’s a big difference. I would be extremely upset, angry and offended if anyone said that about me. We are all people first and foremost, and sometimes that seems to get forgotten. Okay, I am kept alive by my tube, but I’m also kept alive by my inhalers, and you don’t see people going around saying “I love an asthmay”.
I may be being a hypocrit, as I have done publicity about life on TPN, but that was in the context of my life goals and aims, and was done in part to help PINNT, who are a fabulous charity that support people who are living on artificial nutrition. I guess it’s different though, as I wasn’t trying to raise awareness as such, just talking about my life, which happens to include TPN.
I don’t want to offend anyone, and I’ve seen some good proactive posts, but I just can’t support the general awareness campaign.